Table of Contents
Recovering the revenue providers and hospitals are owed has always been a challenge but recently claim denials have been having a larger impact in a negative way.
Surveys by various groups are pointing to the fact that providers are feeling the pinch of those denied claims. Adonis polled more than 120 leaders across 18 specialties and found that 62% of them cited denials and managing underpayments as their top obstacle for revenue growth.
“Denials are no longer just a revenue cycle nuisance, they’re materially impacting provider margins,” said GetixHealth VP of Business Development Elizabeth Allen. “When we’re seeing losses climb past 6% of net revenue on inpatient care, it’s clear that organizations need to shift from reactive recovery to proactive prevention.”
There is hard data to back up that belief. In a recent report, Kodiak Solutions analyzed revenue cycle data for 2,300 hospitals and 350,000 physicians and found that in 2025 providers lost out on 6.6% of net revenue to insurer denials and unpaid patient bills when attempting to collect payments for commercially insured inpatient care. This was up from 5.4% in 2024. On the outpatient side, claims denials and uncollected patient bills increased from 8.9% in 2024 to 10.3% in 2025.
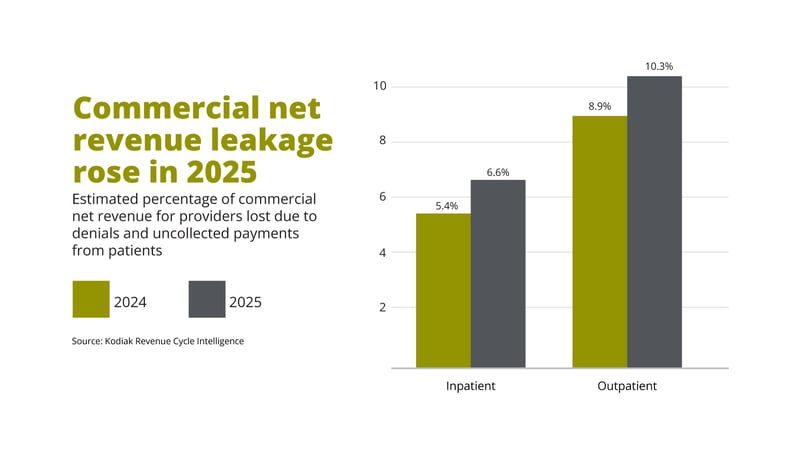
Even though Medicare and Medicaid denial rates are higher overall, commercial insurers tend to pay more, meaning those claims denials have a larger impact on provider revenue.
When you break down the difference in commercial insurer denials, the initial denials were nearly twice as high for inpatient claims vs outpatient claims, which are usually less expensive of the two. The report stated that across all payers, initial and final denial rates for inpatient claims rose more than 12% and 14%, respectively, year-over-year, a significant increase. Add to that, insurers often ask for medical records to justify high-dollar claims and sometimes require additional documentation after the initial request and still deny payment. This burden increases the providers’ workload without increasing the revenue recovery.

Providers are now asking themselves how they can combat this rise in denials without creating an even bigger burden for their staff. Many are looking towards partners that can help not only fix denied claims but also find ways to stop them from happening.
“The challenge isn’t just the volume of denials, it’s the growing complexity behind them. Providers are being asked for more documentation, more follow-ups, and more rework, often without resolution,” said Kimberlee Smallwood, Asst. VP of Operations. “That’s why a structured approach focused on early identification, rapid correction, and root cause analysis is critical.”
There are several steps the right partner can take to help mitigate these issues, including:
- Early detection of problems
- Timely Filing Protection
- Rapid Correction & Resubmission
- Strong Denial Management & Appeals
- Root Cause Analysis
- Automation & AI to reduce missed follow-ups
- Continuous monitoring & reporting
- Close collaboration with the provider
Rising denial rates are challenging providers nationwide, making it critical to have the right strategy—and potentially the right partner—in place. GetixHealth can quickly standup teammates to work in your system to work down denial backlogs. We go beyond prevention, providing dedicated experts who manage denials from cradle to grave, ensuring consistent follow-through to resolution and payment. This approach not only strengthens financial performance but also allows healthcare organizations to prioritize what they do best: caring for patients and allowing us to be "The Core Behind Your Care".


